by Wilton Alston and Dr Shibrah Jamil
Belief is a beautiful armor. But makes for the heaviest sword. Like punching underwater, you never can hit who you’re trying for.
~ John Mayer, “Belief”It’s not the responsibility of the unvaccinated to protect the vaccinated, that’s the vaccine’s job.
~ Unknown
Politicians and media, in lock-step, have claimed that the unvaccinated are the reason the COVID-19 pandemic is not ending, and because of them society cannot return to a normal way of living. Some governing authorities are taking this point-of-view one step further and advocating harsh punitive measures for anyone refusing to be vaccinated, based on this fabricated “pandemic of the unvaccinated.”
Does the foundation of immunology, epidemiology, and ethics, on which medical decisions have historically been made, support this? Does the 10+ months of data accumulated since COVID-19 vaccines were introduced validate the existence of a pandemic of the unvaccinated?
What does it mean to be immune and how does that relate to being vaccinated?
In order to answer these questions and fully grasp the magnitude of the faulty premises on which COVID-19 vaccine policy is being formulated, one needs to have a basic understanding of immunity and how it is achieved.
At a glance:
- Immunity is the body’s ability to resist infection by producing antibodies or a T-cell response after exposure to an infectious agent.
- Vaccines are substances which stimulate the production of an immune response without inducing the disease.
- Vaccination refers to the act of receiving a vaccine.
- Immunity developed to a pathogen subsequent to and as a direct result of receiving the vaccine, is referred to as immunization.
- Immunity is not synonymous with vaccination.
- COVID-19 vaccines have not been shown to result in immunization.
The Centers for Disease Control and Prevention (CDC) currently defines[1] immunity, immunization, vaccine, and vaccination as follows:
Immunity: Protection against a disease[2]. There are two types of immunity, passive and active. Immunity is indicated by the presence of antibodies in the blood and can usually be determined with a laboratory test (this CDC definition is also limited as it does not take into account T-cell mediated or mucosal IgA in the absence of readily detectable antibodies in blood).
Active Immunity: The production of antibodies or a specific T-cell mediated response against a pathogen by the immune system. Active immunity can be acquired in two ways, either by contracting the disease or through vaccination.
Passive Immunity: Protection against disease through antibodies produced by another human being or animal. Passive immunity is effective, but protection is generally limited and diminishes over time (usually a few weeks or months). For example, maternal antibodies are passed to the infant prior to birth. These antibodies temporarily protect the baby for the first 4-6 months of life.
Immunization: The process of being made immune or resistant to an infectious disease, typically by the administration of a vaccine. It implies that an immune response was elicited.
Vaccine: A preparation that is used to stimulate the body’s immune response against diseases. (historically defined as a suspension of live (usually attenuated) or inactivated microorganisms (e.g. bacteria or viruses) or fractions thereof administered to induce immunity and prevent infectious diseases and their sequelae, the CDC recently changed the definition of vaccines in order to accommodate mRNA and DNA therapeutics.)
Vaccination: The physical act of administering any vaccine or toxoid.
The figure below is an idealized model of the path to immunity for an individual.
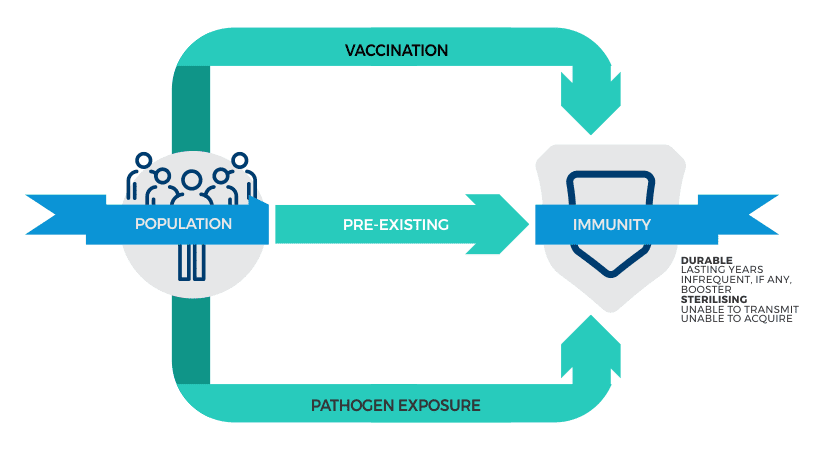
Figure 1: Idealized Routes to Immunity, Pre-COVID
It is clear there are several ways to attain immunity, vaccinations are but one method. Thus the goal of one hundred percent vaccination is misguided. The objective should be to move as many people as possible into the immune group regardless of the route taken to immunity.
If a substantial number of people are already immune to the pathogen, the necessity to vaccinate is reduced. One example that showcases this is the Diamond Princess[3] cruise ship. Data from the ship indicates that up to 80% of people have prior immunity from exposure to closely related Coronaviruses[4] and thus only a small section of the population[5] is at risk of serious illness from SARS-CoV-2, negating the need for vaccination in these individuals. Similarly, if a substantial number of people are immune due to sickness and recovery, the necessity to vaccinate is further reduced.
COVID-19 vaccines do not provide lasting, durable immunity, and in fact, the 6-month follow-up studies of Pfizer and Moderna vaccines show a minor increase in total mortality of the vaccinated group. CDC Director Rochelle Walensky[6] stated in an interview, that “they [the vaccines] continue to work well for Delta, with regard to severe illness and death — they prevent it. But what they can’t do anymore is prevent transmission.” (Emphasis added.) Neither were the vaccines properly tested to determine if they produce this type of immunity[7]. Initial studies, under which EUA was granted, explicitly stated the endpoint measures were PCR test[8] positivity, accompanied by at least one from a list of COVID-19 symptoms.
Peter Hotez, Dean of the National School of Tropical Medicine at Baylor College of Medicine in Houston, cited in “Will Covid-19 vaccines save lives? Current trials aren’t designed to tell us”, says:
Ideally, you want an antiviral vaccine to do two things . . . first, reduce the likelihood you will get severely ill and go to the hospital, and two, prevent infection and therefore interrupt disease transmission.
Peter Doshi, senior editor of the British Medical Journal and associate professor at the University of Maryland School of Pharmacy, adds:
Yet the current phase III trials are not actually set up to prove either. None of the trials currently underway are designed to detect a reduction in any serious outcome such as hospital admissions, use of intensive care, or deaths. Nor are the vaccines being studied to determine whether they can interrupt transmission of the virus.
Statements by the CDC make it clear that the COVID-19 vaccine(s) do not prevent one from getting infected with SARS-Cov-2 or prevent transmission of COVID-19 if an individual acquires it. Furthermore, due to the large number of COVID-recovered[9] individuals, a reasonably high number of people already have immunity and thus have no need to be vaccinated. Numerous studies indicate natural immunity provides equivalent or superior protection to vaccine induced immunity.
Official documents from organizations such as the FDA provide answers to key questions about the performance of the Pfizer vaccine; for example, the following can be found on their FAQ (Frequently Asked Questions) page[10], as of the published date of this article[11]:
Question: What data did FDA evaluate to support Emergency Use Authorization of Pfizer-BioNTech COVID-19 Vaccine in individuals 12 through 15 years of age?
Answer: The effectiveness data to support the EUA in adolescents in this age group is based on immunogenicity and an analysis of COVID-19 cases. …An analysis of cases of COVID-19 occurring among participants 12 through 15 years of age seven days after the second dose was also conducted. In this analysis, among participants without evidence of prior infection with SARS-CoV-2, no cases of COVID-19 occurred among 1,005 vaccine recipients and 16 cases of COVID-19 occurred among 978 placebo recipients; the vaccine was 100% effective in preventing COVID-19. At this time, there is limited data to address whether the vaccine can prevent transmission of the virus from person to person. In addition, at this time data are not available to determine how long the vaccine will provide protection. (Emphasis added)
Question: If a person has received the Pfizer-BioNTech COVID-19 Vaccine or Comirnaty, will the vaccine protect against transmission of SARS-CoV-2 from individuals who are infected despite vaccination?
Answer: Most vaccines that protect from viral illnesses also reduce transmission of the virus that causes the disease by those who are vaccinated. While it is hoped this will be the case, the scientific community does not yet know if the Pfizer-BioNTech COVID-19 Vaccine will reduce such transmission.
According to these official statements from the governmental body that approved the vaccine for widespread use, and the most recent medical studies, the data provides overwhelming evidence that vaccines do not prevent transmission. In fact, emergent data suggests that the vaccinated are not able to provide sufficient protection against the spread of COVID-19 generally. According to a recent Lancet[12] article, “It appears to be grossly negligent to ignore the vaccinated population as a possible and relevant source of transmission when deciding about public health control measures.”
The length of limited protection – the durability of the immunity – is also unknown. Using the CDC definitions, it is clear that the vaccines do not confer the type of protection that we are accustomed to expecting from what we heretofore characterized as “a vaccine.” The COVID-19 therapies do not result in meaningful immunity, nor do they prevent the recipient from subsequently passing the infection on to someone else. At best then, the COVID-19 vaccine(s) results in a situation modeled in Figure 2 below.
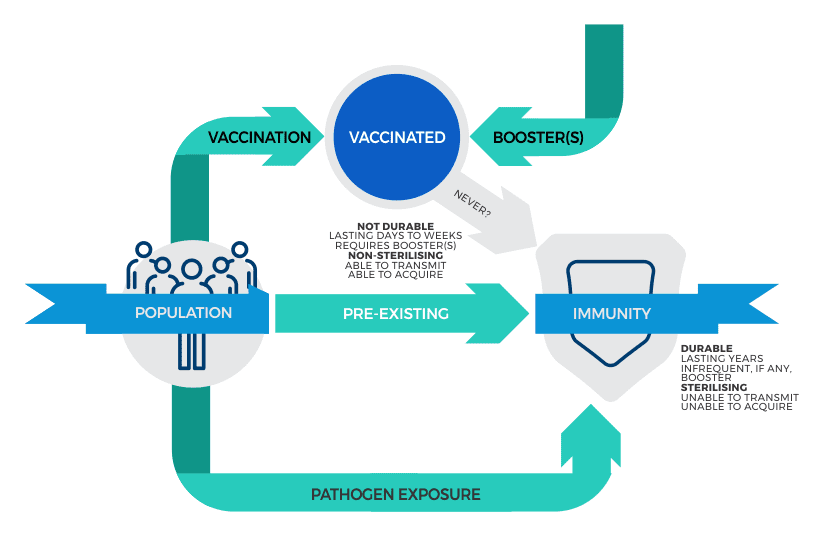
Figure 2: Actual Routes to Vaccinated versus Routes to Immunity
Mandates cannot be justified when the COVID-19 vaccines being used provide neither durable nor sterilizing immunity. Furthermore, immunity, as defined by the CDC, can be obtained via other routes without the negative side-effects associated with the experimental, poorly-tested[13] vaccines that are based on novel gene therapy. Multiple studies have shown people who have recovered are no worse off[14] than those who have been vaccinated, and may actually be better off. We also know that non-vaccinated persons, naturally immune or not, present no danger[15] to anyone if not they are healthy. Studies also show that people with naturally-acquired immunity do not benefit[16] further from vaccination. As recently as September 12, 2021, statistics out of the UK[17] indicate worse outcomes in vaccinated individuals[18] compared to those who are vaccine-free, i.e., have received no injections at all. Of the total deaths recorded in the UK for the Delta variant for the September 17, 2021 Technical Briefing, 28.4% were unvaccinated, 6.5% were partially vaccinated, and 63.5% were fully vaccinated[19], with 1.6% having unknown vaccination status. Studies have confirmed that vaccinated individuals still have viral loads[20, 21] similar to individuals who are unvaccinated.
Again we ask, what justification is there for mandating vaccines for anyone, and particularly for those who have recovered? Why is the “vaccination spin cycle,” as depicted in the figures above, being celebrated at the cost of attacking those who are already immune? We know individuals who are not immune to SARS-CoV-2 are only a risk to themselves and pose no risk to those who are immune, or who should be immune, given their inoculation with a vaccine! There is NO logical basis or scientific theory for the vaccinated to blame the unvaccinated for anything, aside from the human tendency to look for a scapegoat, which is heavily promoted by the mainstream media. “Blame the unvaccinated” is giving rise to a new form of segregation; categorizing people as either “vaccinated” or “unvaccinated” is identical to discrimination witnessed historically to disenfranchise a particular group of people. As pointed out in the Lancet by a commentator from Germany:
It is therefore wrong and dangerous to speak of a pandemic of the unvaccinated. Historically, both the USA and Germany have engendered negative experiences by stigmatising parts of the population for their skin colour or religion. I call on high-level officials and scientists to stop the inappropriate stigmatisation of unvaccinated people, who include our patients, colleagues, and other fellow citizens, and to put extra effort into bringing society together.
COVID-19 vaccines designed using novel mRNA technology are largely untested and were introduced into general use with limited safety and efficacy data and studies, which, to date, have not been completed. The pharmaceutical companies’ own published data raises more questions than it answers. Therefore it is reasonable for people to have questions and be cautious about rushing to get vaccinated. However, if one believes the COVID-19 vaccinations are doing the job they were designed to do, then once a person is vaccinated, they have to believe they are protected. Once you are vaccinated and believe you have vaccine protection, do unvaccinated individuals present a danger to you? There are but two options:
- The vaccine(s) work, so the vaccinated person is safe and does not need to worry about the unvaccinated.
- The vaccine(s) do not work, so the vaccinated and unvaccinated pose the same risk to each other.
Prior to the current pandemic, had you ever wondered if the person standing next you was vaccinated against the flu? Or, for that matter, any other disease? Let us assume, just for argument’s sake, that one attempts to justify the vaccination mandate on the same basis as existing and widespread mandates for wearing a motorcycle helmet or seatbelts. The problem with that justification is this. Wearing a seatbelt has clear benefits, and provides no potential harm to the wearer. There is no cost, all benefits. Furthermore, violating these mandates results in minor fines and no other long lasting repercussions. COVID-19 vaccines carry risk, as all medical interventions do. National databases appear to show very strong adverse event signals. Hence, there is cost in the short term, and any potential long term cost is unknown. Wearing a simple device simply cannot be compared to a forced, invasive medical treatment.
In the end, it is neither the unvaccinated nor the vaccinated who are the reason for this never-ending global crisis. It is the deployment of a militarized, coercive, and monetized strategy to handle a medical emergency, by governments around the world, with an overemphasis on the role of a vaccination in ending the pandemic, and implementation of draconian and ineffective measures to achieve the goal of one hundred percent global vaccination. This approach has marginalized practitioners in the medical field and community who were best positioned to lead the fight against the virus, and has also destroyed much of society’s faith in public health.
Appropriate medical solutions would allow SARS-CoV-2 to be treated much like we do other common Coronaviruses, especially in view of the evolution into milder strains, which is usual, expected, and appears to be occurring with this virus. In the absence of elimination (which is unrealistic), it will surely become a virus that is so widely-prevalent that it poses little threat to anyone. The current approach, and the narratives that support it, seem to be aimed at achieving exactly the opposite of this, which appears to aim to prolong the extent and impact of the COVID-19 pandemic.
References
- These definitions were recently revised, apparently in response to the need to promote widespread vaccination.
- We find the CDC’s definition to be incorrect. Factually, immunity is the response of the immune system to an antigen which should provide protection against a disease. A disease may or may not ensue.
- Diamond Princess Mysteries – Watts Up With That?
- Cross-reactive CD4+ T cells enhance SARS-CoV-2 immune responses upon infection and vaccination | medRxiv
- Eurosurveillance | Descriptive study of COVID-19 outbreak among passengers and crew on Diamond Princess cruise ship, Yokohama Port, Japan, 20 January to 9 February 2020
- Fully vaccinated people who get a Covid-19 breakthrough infection can transmit the virus, CDC chief says – CNN
- Peter Doshi: Pfizer and Moderna’s “95% effective” vaccines—let’s be cautious and first see the full data – The BMJ
- Table 1 Reported COVID-19 vaccine efficacy data from phase III trials (nature.com)
- Covid-19: Do many people have pre-existing immunity?
- Pfizer-BioNTech COVID-19 Vaccine Frequently Asked Questions | FDA
- The FDA (and CDC) have been somewhat aggressive in modifying their websites as the political winds change, so it is possible that these words will be modified from what is shown above by the time this article is published or at some point thereafter!
- https://www.thelancet.com/journals/lanepe/article/PIIS2666-7762(21)00258-1/fulltext?s=08#%20
- Peter Doshi: Pfizer and Moderna’s “95% effective” vaccines—we need more details and the raw data – The BMJ
- Necessity of COVID-19 vaccination in previously infected individuals | medRxiv
- Position Paper The Science And The Ethics Regarding The Risk Posed By Non-Vaccinated Individuals
- Comparing SARS-CoV-2 natural immunity to vaccine-induced immunity: reinfections versus breakthrough infections | medRxiv
- SARS-CoV-2 variants of concern and variants under investigation (publishing.service.gov.uk)
- an epidemic of the vaccinated – by el gato malo – bad cattitude (substack.com)
- In this case, “fully-vaccinated” means greater than 14 days post dose 2 of multi-dose vaccine.
- Outbreak of SARS-CoV-2 Infections, Including COVID-19 Vaccine Breakthrough Infections, Associated with Large Public Gatherings — Barnstable County, Massachusetts, July 2021 | MMWR (cdc.gov)
- Shedding of Infectious SARS-CoV-2 Despite Vaccination
Additional References
Compiled by: R. Iván Iriarte, MD, MS
Infection Fatality Rate
- Ioannidis, PA. The infection fatality rate of COVID-19 inferred from seroprevalence data. Bulletin of the WHO. July 14, 2020. https://www.medrxiv.org/content/10.1101/2020.05.13.20101253v3
- Ioannidis, PA. The infection fatality rate of COVID-19 inferred from seroprevalence data. Bulletin of the WHO. 2021; 99:19-33. https://www.who.int/bulletin/volumes/99/1/20-265892.pdf
- Axfors, C. Ioannidis, PA. Infection fatality rate of COVID-19 in community-dwelling populations with emphasis on the elderly: An overview. https://www.medrxiv.org/content/10.1101/2021.07.08.21260210v2
- Ioannidis, PA. Reconciling estimates of global spread and infection fatality rates of COVID-19: An overview of systematic evaluations. Eur J Clin Invest. 2021; 51:e13554. https://doi.org/10.1111/eci.13554
Previous Immunity
A high percentage of the population has previous immunity to SARS-CoV-2, through cell-mediated immunity. Probably this is due from exposure in the past to other coronaviruses, and a phenomenon vastly known for decades, called cross-immunity.
- Bonifacius, A. et al. COVID-19 immune signatures reveal stable antiviral T cell function despite declining humoral responses. Immunity. 54, 340-354, 2021. https://doi.org/10.1016/j.immuni.2021.01.008
- Doshi, P. (Ed). Covid-19: Do many people have pre-existing immunity? BMJ. 2020; 370:m3563 https://www.bmj.com/content/370/bmj.m3563
- Echeverría G. et al. Pre-existing T-cell immunity to SARS-CoV-2 in unexposed healthy controls in Ecuador, as detected with a COVID-19 Interferon-Gamma Release Assay. International Journal of Infectious Diseases. (2021). https://doi.org/10.1016/j.ijid.2021.02.034
- Le Bert, N. et al. Different pattern of pre-existing SARS-COV-2 specific T cell immunity in SARS-recovered and uninfected individuals. (2020). https://doi.org/10.1101/2020.05.26.115832
- Tarke A. et al. Comprehensive analysis of T cell immunodominance and immunoprevalence of SARS-CoV-2 epitopes in COVID-19 cases. Cell Reports Medicine 2, February 16, 2021. https://pubmed.ncbi.nlm.nih.gov/33521695/
- Swadling, L. et al. Pre-existing polymerase-specific T cells expand in abortive seronegative SARS-CoV-2. Nature (2021). https://www.nature.com/articles/s41586-021-04186-8
Asymptomatic Transmission
Asymptomatic transmission of an infectious disease is very rare, and never the driver of an epidemic. There is no reason to think that it would be different with COVID, and the data supports this statement.
- Fauci, A.
- Patrozou, E. Mermel, LA. Does Influenza Transmission Occur from Asymptomatic Infection or Prior to Symptom Onset? Public Health Reports. 2009. Vol 124. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2646474/pdf/phr124000193.pdf
- Gao, M. et al. A study on infectivity of asymptomatic SARS-CoV-2 carriers. Respiratory Medicine 169 (2020) 106026. https://www.resmedjournal.com/article/S0954-6111(20)30166-9/fulltext
- Madewell, Z. et al. Household Transmission of SARS-CoV-2: A Systematic Review and Meta-analysis. JAMA Network Open. 2020; 3(12). https://jamanetwork.com/journals/jamanetworkopen/fullarticle/2774102
- Pollock, AM., Lancaster, J. Asymptomatic Transmission of COVID-9. BMJ 2020;371
https://www.bmj.com/content/371/bmj.m4851 - Cao, S et al. Post-lockdown SARS-CoV-2 nucleic acid screening in nearly ten million residents of Wuhan, China. Nature Communications. (2020) 11:5917. https://www.nature.com/articles/s41467-020-19802-w
Problems with PCRs
PCRs yield a very high percentage of false positive results, especially in asymptomatic individuals. This is consistent with a previously well-known concept of Epidemiology, which has to do with the low positive predictive value of tests done in asymptomatic individuals. The concept is demonstrated in studies done with the PCR for SARS-CoV-2. There have also been serious problems identified with the manner in which this particular PCR test was developed and authorized for use. For some reason, authorities persist in doing this test in asymptomatic individuals, and using it as criterion for defining a “case”, quarantining individuals, and restricting access to services or places. This test (and other tests) should be used exclusively by physicians as a diagnostic aid in sick individuals.
- Cohen, A. N., & Kessel, B. (2020, May 20). False positives in reverse transcription PCR testing for SARS-CoV-2. https://www.medrxiv.org/content/10.1101/2020.04.26.20080911v2
- Cohen, A. N., & Kessel, B., Milgroom, M. (2020, August). Diagnosing COVID-19 infection: the danger of over-reliance on positive test results https://www.medrxiv.org/content/10.1101/2020.04.26.20080911v4
- Surkova E. False Positive Results (2020). https://www.thelancet.com/pdfs/journals/lanres/PIIS2213-2600(20)30453-7.pdf
- Bullard, J. et al. Predicting Infectious Severe Acute Respiratory Syndrome Coronavirus 2 from Diagnostic Samples. Clinical Infectious Diseases. 2020: 71 (15 November). https://academic.oup.com/cid/article/71/10/2663/5842165
- Dahdouh, E. et al. Ct values from SARS-CoV-2 diagnostic PCR assays should not be used as direct estimates of viral load. Journal of Infection. 2020. October 24. https://pubmed.ncbi.nlm.nih.gov/33131699/
- Jaafar, R. Aherfi, S. Wurtz, N. Grimaldier, C Hoang, VT. Colson, P. Raoult, D. La Scola, B. Correlation Between 3790 Quantitative Polymerase Chain Reaction–Positives Samples and Positive Cell Cultures, Including 1941 Severe Acute Respiratory Syndrome Coronavirus 2 Isolates. Clinical Infectious Diseases. 29 September, 2020. https://doi.org/10.1093/cid/ciaa1491
- Jefferson, T., & Heneghan, G. el al. (2020) Are you infectious if you have a positive PCR test for COVID-19? https://www.cebm.net/covid-19/infectious-positive-pcr-test-result-covid-19/
- Santos, Chiesa. PCR Positives. What Do They Mean? (Sept. 2020) https://www.cebm.net/wp-content/uploads/2020/09/PCR-test-Infectivity-Sep-2020.pdf
- WHO. Information notice for IVD Users 2020/05 (2021). https://www.who.int/news/item/20-01-2021-who-information-notice-for-ivd-users-2020-05
- Gnomegen COVID-19 Digital PCR Detection Kit. Instructions for Use. P. 15. https://www.fda.gov/media/137895/download
- LBL-0109-04-900251-EUA-CE-Smart-Detect (P. 26). http://i8sit3w4v3z1h99oi1gmrx61-wpengine.netdna-ssl.com/wp-content/uploads/2020/10/LBL-0109-05-900251-EUA-CE-Smart-Detect-SARS-CoV-2-rRT-PCR-Kit-Package-Insert.pdf
- Corman-Drosten Review Report. https://cormandrostenreview.com/report/
Overdiagnosis of COVID in Hospitalization and Mortality Statistics
There is much evidence demonstrating that hospitalization and mortality rates from COVID-19 have been grossly overestimated in most countries, basing estimates solely on testing with PCRs, disregarding clinical criteria.
- https://www.msn.com/en-us/health/medical/over-half-of-covid-hospitalisations-tested-positive-post-admission/ar-AAMChoj?fbclid=IwAR09GuYb4_w_Z4MwT5u6QCFWuwSizegsv866wTmlLRVyeBA-pbm5R2oLyHk
- Vital Statistics Reporting Guidance. Guidance for Certifying Deaths Due to Coronavirus Disease 2019 (COVID–19). Report No. 3. April 2020. https://www.cdc.gov/nchs/data/nvss/vsrg/vsrg03-508.pdf
- McGowan, J. Are COVID Death Rates Comparing Apples and Oranges? Mathematical Software. January 25, 2021. http://wordpress.jmcgowan.com/wp/are-covid-death-numbers-comparing-apples-and-oranges/
Masks
All important scientific literature, and even guidelines previously published by the WHO and CDC irrevocably state that masks are not effective reducing community transmission of COVID-19, or any viral respiratory disease.
- Association of American Physicians and Surgeons. Mask Facts. September 2020. https://aapsonline.org/mask-facts/
- Bundgaard, H., Bundgaard, JS. Effectiveness of Adding a Mask Recommendation to other Public Health Measures to Prevent SARS-CoV-2 Infections in Danish Mask Wearers. Annals of Internal Medicine. 2020 Nov 18. https://www.acpjournals.org/doi/10.7326/M20-6817
- Meehan, J. An Evidence Based Scientific Analysis of Why Masks are Ineffective, Unnecessary, and Harmful. November, 2020. https://www.meehanmd.com/articles/post/173679/an-evidence-based-scientific-analysis-of-why-masks-are-ineffective-unnecessary-and-harmful
- Swiss Policy Research: Are Face Masks Effective? The Evidence (October 25, 2020). https://swprs.org/face-masks-evidence/
- Xiao, J. et al. Nonpharmaceutical Measures for Pandemic Influenza in Nonhealthcare Settings—Personal Protective and Environmental Measures. CDC PolicyReview. Vol 26:5. May, 2020 https://wwwnc.cdc.gov/eid/article/26/5/19-0994_article?fbclid=IwAR1wgGi1n82n8eGLEFTIbzV3atyHqop9DqK-rhx7itJ0SY3eZm5erwTZw6g
- WHO. Mask use in the context of COVID-19. Interim guidance. 1 December 2020. https://www.who.int/publications/i/item/advice-on-the-use-of-masks-in-the-community-during-home-care-and-in-healthcare-settings-in-the-context-of-the-novel-coronavirus-(2019-ncov)-outbreak
- Horowitz, D. Comprehensive analysis of 50 states shows greater spread with mask mandates. https://www.theblaze.com/op-ed/horowitz-comprehensive-analysis-of-50-states-shows-greater-spread-with-mask-mandates
- Rosner, E. Adverse Effects of Prolonged Mask Use among Healthcare Professionals during COVID-19. Journal of Infectious Disease Epidemiology. 2020, 6:130. https://clinmedjournals.org/articles/jide/journal-of-infectious-diseases-and-epidemiology-jide-6-130.php?jid=jide
- Schwarz, S. et al. Corona children studies “Co-Ki”: First results of a Germany-wide registry on mouth and nose covering (mask) in children. https://doi.org/10.21203/rs.3.rs-124394/v2
- Techasatian, L. et al. The Effects of the Face Mask on the Skin Underneath: A Prospective Survey During the COVID-19 Pandemic. Journal of Primary Care and Community Health. 2020. 11: 1-7. https://journals.sagepub.com/doi/10.1177/2150132720966167
- Dingwall, R. COVID Science and Politics – the Case of Face Masks. https://www.socialsciencespace.com/2021/08/covid-science-and-politics-the-case-of-face-masks/
- Guerra, DD and Guerra, DJ. Mask mandate and use efficacy for COVID-19 containment in US States. International Research Journal of Public Health (2021), 5:55. https://escipub.com/irjph-2021-08-1005/
- Alexander, PE. The CDC’s Mask Mandate Study: Debunked. https://www.aier.org/article/the-cdcs-mask-mandate-study-debunked/
- Members of EU Parliament oppose mask mandates. https://odysee.com/@Fingerbob:c/BREAKING-EU-PARLEMENT-OPPOSES-VACCINE-MANDATE-AGENDA:4
Ivermectin
There is enough evidence to support that Ivermectin is an effective medication to treat patients with early symptoms of COVID-19.
- Kory, Pierre et al. Review of the Emerging Evidence Demonstrating the Efficacy of Ivermectin in the Prophylaxis and Treatment of COVID-19. American Journal of Therapeutics: May/June 2021 – Volume 28:3:p e299-e318. https://journals.lww.com/americantherapeutics/Fulltext/2021/06000/Review_of_the_Emerging_Evidence_Demonstrating_the.4.aspx
- McCullough PA, Kelly RJ, Ruocco G, et al. Pathophysiological Basis and Rationale for Early Outpatient Treatment of SARS-CoV-2 (COVID-19) Infection. Am J Med. 2021;134(1):16-22. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7410805/
- Bryant A, Lawrie TA, Dowswell T, et al. Ivermectin for Prevention and Treatment of COVID-19 Infection: A Systematic Review, Meta-analysis, and Trial Sequential Analysis to Inform Clinical Guidelines. Am J Ther. 2021;28(4):e434-e460. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8248252/
COVID in Children
COVID-19 does not affect children in any significant way. Children tend to have very mild symptoms or no symptoms at all from being infected with this virus. Neither do they tend to be highly infectious to others. There are many other respiratory agents that affect children to a higher degree.
- Lee, B. et al. COVID-19 Transmission and Children: The Child is Not to Blame. Pediatrics August 2020, 146 (2) e2020004879; https://doi.org/10.1542/peds.2020-004879
- Ludvigsson, J. et al. Open Schools, Covid-19, and Child and Teacher Morbidity in Sweden. February 18, 2021. https://www.nejm.org/doi/full/10.1056/NEJMc2026670
- Wood, R. et al. Sharing a household with children and risk of COVID-19: a study of over 300,000 adults living in healthcare worker households in Scotland. https://www.medrxiv.org/content/10.1101/2020.09.21.20196428v2
- Child mortality and COVID-19. May, 2021. https://data.unicef.org/topic/child-survival/covid-19/
- Children and COVID-19: State-Level Data Report. October, 2021. https://www.aap.org/en/pages/2019-novel-coronavirus-covid-19-infections/children-and-covid-19-state-level-data-report/
- Provisional Death Counts for Coronavirus Disease 2019 (COVID-19). August 2021. https://www.cdc.gov/nchs/nvss/vsrr/covid_weekly/index.htm
Vaccination in Children
The risk of myocarditis and other adverse effects from COVID-19 vaccination in children is considerable. With a very low risk of infection in children, it seems absurd to justify vaccinating children against COVID-19.
- Høeg, TB. Et al. SARS-CoV-2 mRNA Vaccination-Associated Myocarditis in Children Ages 12-17: A Stratified National Database Analysis. https://www.medrxiv.org/content/10.1101/2021.08.30.21262866v1
- https://pandata.org/covid-vaccine-for-children-risks/
- Rogers, T. Pfizer COVID Vaccine Fails Risk-Benefit Analysis in Children 5 to 11. https://childrenshealthdefense.org/defender/fda-pfizer-covid-vaccine-risk-benefit-analysis-nntv-children/
- Chua, GT. et al. Epidemiology of Acute Myocarditis/Pericarditis in Hong Kong Adolescents Foollowing Comirnaty Vaccination. Clinical Infectious Diseases. 28 November, 2021. https://academic.oup.com/cid/advance-article-abstract/doi/10.1093/cid/ciab989/6445179
- Patone, M. et al. Risks of myocarditis, pericarditis, and cardiac arrhythmias associated with COVID-19 vaccination or SARS-CoV-2 infection. Nature Medicine. 2021. https://www.nature.com/articles/s41591-021-01630-0
- Comment: https://vinayprasadmdmph.substack.com/p/uk-now-reports-myocarditis-stratified?justPublished=true
Vaccination in General
The reports and probability of serious adverse events from the COVID-19 vaccine cannot be ignored. These become even more important when the biological mechanisms by which these products act are considered, and the lack of sufficient data from short term clinical trials and experience. Considering compulsory vaccinations – under any circumstances – but even more under these circumstances, is unacceptable. Vaccinated individuals can become infected and may transmit the infection equally to unvaccinated individuals. Unvaccinated individuals, if they are not sick, pose no risk to the population. The more vaccines, the higher risk for new infections.
- https://www.openvaers.com/covid-data
- https://www.openvaers.com/covid-data/mortality
- The Israeli Public Emergency Council for the COVID-19 Crisis. Position Paper. The Science and the Ethics Regarding the Risk Posed by Non-Vaccinated Individuals. https://pecc-il.org/docs/position-paperthe-science-and-the-ethics-regarding-the-risk-posed-by-non-vaccinated-individuals/?fbclid=IwAR34_1WysslUWKhgP8Q3UPVbpjyz5AU1mFWmZX9_D4
- Pollack, FP. Et al. Safety and Efficacy of the BNT162b2 mRNA Covid-19 Vaccine https://pubmed.ncbi.nlm.nih.gov/33301246/
- Olifaro, P. et al. COVID-19 vaccine efficacy and effectiveness—the elephant (not) in the room. https://www.thelancet.com/journals/lanmic/article/PIIS2666-5247(21)00069-0/fulltext
- https://rumble.com/vk5zfm-dr.-peter-mccullough-urgent-warning-about-poisonous-jabs-an-agonizing-situa.html?fbclid=IwAR3qrJj5Txk7NZFvEoCzylB9TA5jFAS2_iOJak4dCWZc5GItqY5nGeN6ayU
- https://rairfoundation.com/warning-renowned-virologist-sucharit-bhakdi-warns-against-hastily-created-gene-altering-coronavirus-vaccine-video/
- Riemersma, KK. Et al. Shedding of Infectious SARS-CoV-2 Despite Vaccination. August 24, 2021. https://www.medrxiv.org/content/10.1101/2021.07.31.21261387v4.full.pdf
- Classen, JB. US COVID-19 Vaccines Proven to Cause More Harm than Good Based on Pivotal Clinical Trial Data Analyzed Using the Proper Scientific Endpoint, “All Cause Severe Morbidity”. Trends Int Med. 2021; 1(1): 1-6. https://www.scivisionpub.com/pdfs/us-covid19-vaccines-proven-to-cause-more-harm-than-good-based-on-pivotal-clinical-trial-data-analyzed-using-the-proper-scientific–1811.pdf
- https://truthbasedmedia.com/2021/08/21/two-top-virologists-frightening-warnings-about-covid-injections-ignored-by-government-and-big-media/
- https://basedunderground.com/2021/09/03/ultra-vaxxed-booster-heavy-israel-now-has-more-covid-infections-per-capita-than-any-country-in-the-world/
- Vogel G. et al. American Association for the Advancement of Science. https://www.sciencemag.org/news/2021/06/israel-reports-link-between-rare-cases-heart-inflammation-and-covid-19-vaccination
- http://portal.unesco.org/en/ev.php-URL_ID=31058&URL_DO=DO_TOPIC&URL_SECTION=201.html
- Subramanian, SV. Et al. Increases in COVID‑19 are unrelated to levels of vaccination across 68 countries and 2947 counties in the United States. European Journal of Epidemiology. September, 2021. https://link.springer.com/content/pdf/10.1007/s10654-021-00808-7.pdf
- Delepine, G. Covid-19 Vaccines Lead to New Infections and Mortality: The Evidence is Overwhelming. https://www.globalresearch.ca/covid-19-vaccines-lead-to-new-infections-and-mortality-the-evidence/5746393
- Kampf, G. COVID-19: Stigmatising the unvaccinated is not justified. The Lancet. Vol 398:10314. P. 1871. November 20, 2021. https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(21)02243-1/fulltext#back-bib1
- Gundry, SR. Mrna COVID Vaccines Dramatically Increase Endothelial Inflammatory Markers and ACS Risk as Measured by the PULS Cardiac Test: a Warning. 8 Nov 2021 2021; 144: A10712. https://www.ahajournals.org/doi/10.1161/circ.144.suppl_1.10712
- Salvatore, P. et al. Transmission potential of vaccinated and unvaccinated persons infected with the SARS-CoV-2 Delta variant in a federal prison, July—August 2021. https://www.medrxiv.org/content/10.1101/2021.11.12.21265796v1
- Hirsh, H. Bradley, G. Covid-19 Vaccine Mandates Fail the Jacobson Test. November 30, 2021. https://brownstone.org/articles/covid-19-vaccine-mandates-fail-the-jacobson-test/
- Kampf, G. The epidemiological relevance of the COVID-19-vaccinated population is increasing. The Lancet. November 19, 2021. https://www.thelancet.com/journals/lanepe/article/PIIS2666-7762(21)00258-1/fulltext?s=08#%20
- Lyons-Weber, J. In the United States, Vaccination Rates Are Associated with Increased Rate of Spread of SARS-CoV-2, But Not How They Should Be. https://popularrationalism.substack.com/p/in-the-united-states-vaccination
- Beattie, K. Worldwide Bayesian Causal Impact Analysis of Vaccine Administration on Deaths and Cases Associated with COVID-19: A BigData Analysis of 145 Countries. https://www.researchgate.net/publication/356248984_Worldwide_Bayesian_Causal_Impact_Analysis_of_Vaccine_Administration_on_Deaths_and_Cases_Associated_with_COVID-19_A_BigData_Analysis_of_145_Countries
Vaccination in Pregnancy
A study published in NEJM in June, 2021 declares COVID-19 vaccines as safe during pregnancy. Further revisions of this study and article published in November, 2021 demonstrate the limitations and errors of this study and show the high rate of spontaneous abortions in women exposed to the vaccine during their first trimester of pregnancy.
- Shimabukuro TT, Kim SY, Myers TR, et al. 2021. Preliminary findings of mRNA Covid-19 vaccine safety in pregnant persons. New England Journal of Medicine 384(24): 2273–82. https://www.nejm.org/doi/full/10.1056/nejmoa2104983
- Brock AR, Thornley, S. Spontaneous Abortions and Policies on COVID-19 mRNA Vaccine Use During Pregnancy. Science, Public Health Policy and the Law Volume 4:130–143 November, 2021.
https://cf5e727d-d02d-4d71-89ff-9fe2d3ad957f.filesusr.com/ugd/adf864_2bd97450072f4364a65e5cf1d7384dd4.pdf
Natural Immunity
There can be absolutely no doubt that natural immunity from acquiring an infection with SARS-CoV-2 is vastly superior to immunity provided by vaccination. Recommending that those who already have been infected with SARS-CoV-2 to receive the vaccine goes against any rational medical practice.
- Girardot, M. Natural immunity vs Covid-19 vaccine-induced immunity. June 28, 2021. https://www.biznews.com/health/2021/06/28/covid-19-vaccine-immunity
- Murchu, E. et al. Quantifying the risk of SARS‐CoV‐2 reinfection over time. May 18, 2021.
https://onlinelibrary.wiley.com/doi/10.1002/rmv.2260 - Radbruch A. et al. A long term perspective on immunity to COVID. Nature. Vol 595. July 15, 2021.
- Abu-Raddad, LJ. Et al. SARS-CoV-2 antibody-positivity protects against reinfection for at least seven months with 95% efficacy. May 1, 2021. EClinicalMedicine 35 (2021) 100861. https://www.thelancet.com/journals/eclinm/article/PIIS2589-5370(21)00141-3/fulltext
- Haveri, A. et al. Persistence of neutralizing antibodies a year after SARS-CoV-2 infection in humans. European Journal of Immunology. September 27, 2021. https://doi.org/10.1002/eji.202149535
- Gazit, S et al. Comparing SARS-CoV-2 natural immunity to vaccine-induced immunity: reinfections versus breakthrough infections. August 25, 2021. https://www.medrxiv.org/content/10.1101/2021.08.24.21262415v1.full-text
- Shrestha, NK. Et al. Necessity of COVID-19 vaccination in previously infected individuals. August 24, 2021. https://www.medrxiv.org/content/10.1101/2021.06.01.21258176v3
- Cohen, KW. Et al. Longitudinal analysis shows durable and broad immune memory after SARS-CoV-2 infection with persisting antibody responses and memory B and T cells. Cell Reports Medicine. July 21, 2021. https://www.cell.com/cell-reports-medicine/fulltext/S2666-3791(21)00203-2#%20
- Israel, A. et al. Large-scale study of antibody titer decay following BNT162b2 mRNA vaccine or SARS-CoV-2 infection. August 22, 2021. https://www.medrxiv.org/content/10.1101/2021.08.19.21262111v1
- https://www.theblaze.com/amp/horowitz-15-studies-that-indicate-natural-immunity-from-prior-infection-is-more-robust-than-the-covid-vaccines-2654789339?__twitter_impression=true
- https://www.nih.gov/news-events/news-releases/t-cells-recognize-recent-sars-cov-2-variants
- AD Redd et al. CD8+ T cell responses in COVID-19 convalescent individuals target conserved epitopes from multiple prominent SARS-CoV-2 circulating variants. Open Forum Infectious Diseases DOI: 10.1093/ofid/ofab143 (2021).
Lockdowns
Lockdowns cause a lot of harm to the community, and include no discernible benefits.
- AIER (American Institute of Economic Research). Lockdowns Do Not Control the Coronavirus: The Evidence. https://www.aier.org/article/lockdowns-do-not-control-the-coronavirus-the-evidence/
- COVID-19 Alternative Strategy: A Case for Health and Socioeconomic Wellbeing (2020). https://www.aier.org/wp-content/uploads/2020/11/covid_recovery_ireland_white_paper_-_17th_nov.pdf
- https://brownstone.org/articles/more-than-400-studies-on-the-failure-of-compulsory-covid-interventions/
- Chaudhry, R. et al. A country level analysis measuring the impact of government actions, country preparedness and socioeconomic factors on COVID-19 mortality and related health outcomes. EClinicalMedicine 25 (2020) 100464. https://www.thelancet.com/journals/eclinm/article/PIIS2589-5370(20)30208-X/fulltext
- Great Barrington Declaration: https://gbdeclaration.org/
- Johnston, L. UK lockdown was a ‘monumental mistake’ and must not happen again – Boris scientist says (2020). https://www.express.co.uk/life-style/health/1320428/Coronavirus-news-lockdown-mistake-second-wave-Boris-Johnson
- Kulldorff, M. American Institute of Economic Research (2020). https://www.aier.org/article/twelve-principles-of-public-health/
- McClintock, T. Lockdowns are killing us. Mountain Democrat. February, 2021. https://www.mtdemocrat.com/opinion/guest-column-lockdowns-are-killing-us/
- Meunier, T. Full lockdown policies in Western Europe countries have no evident impacts on the COVID-19 epidemic (2020). https://www.medrxiv.org/content/10.1101/2020.04.24.20078717v1
- Norway ‘could have controlled infection without lockdown’: health chief. https://www.thelocal.no/20200522/norway-could-have-controlled-infection-without-lockdown-health-chief
- Schneider, P. Canadian Health Expert: Cost of Lockdowns are at least 10 times higher than benefits. January 15, 2021. https://phillipschneider.com/canadian-health-expert-costs-of-lock-downs-are-at-least-10-times-higher-than-the-benefits/
- PanData: https://pandata.org/
- PANDA. Protocol for reopening society. December, 2020. https://pandata.org/about/protocol-for-reopening-society/




