by Dr David Bell
There was a time when medical publishing went beyond advertising and attempted to uphold the value of objectivity and evidence. The Journal of the American Medical Association (JAMA) was an example of such. JAMA has also become a prime example of their ‘new normal’, being at the forefront of the course reversal of the past 2 years.
The journal pilloried senior doctors for following orthodox public health principles rather than popular opinion, even running articles that echoed Nazi- or phrenology-inspired public health in suggesting medically-trained people whose interpretations differed from those in JAMA were neurologically-impaired. This is behaviour that would have been viewed as appalling just 3 years ago.
Now an obvious and embarrassing failure of non-pharmaceutical interventions and mandated vaccination at Cornell University (all the lockdown and pharmaceutical industry could throw at it) is packaged to promote more of the same, rather than an opportunity to sit back and contemplate whether previous but discarded wisdom in public health may have just been right.
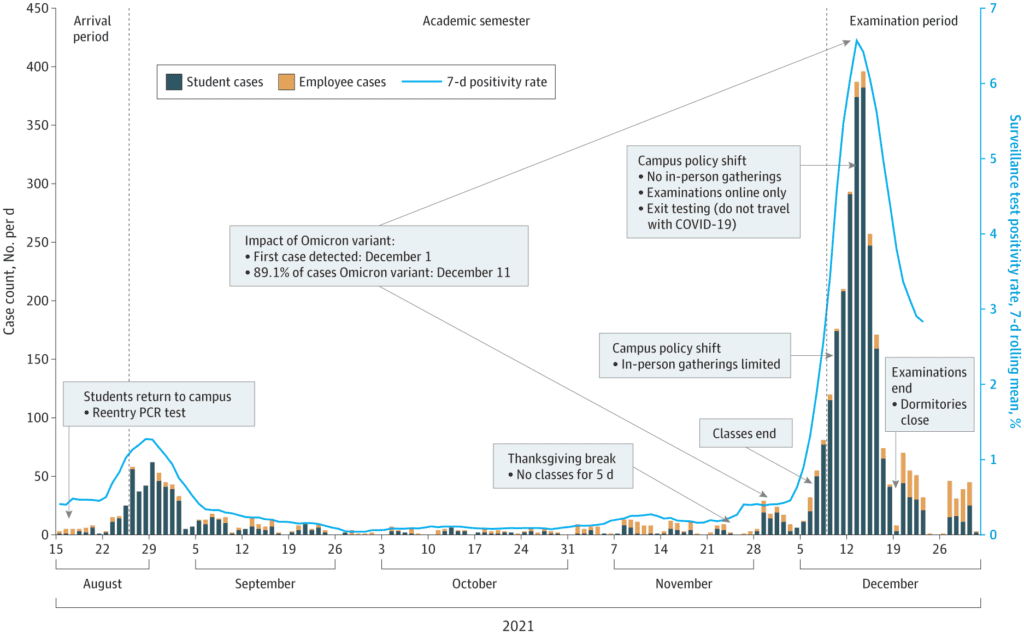
Meredith et al (JAMA,, May 18, 2022) report what can only be described in previous parlance as a mass failure of coerced vaccination and mandated masking and distancing – measures that have been shown to have significant mental and/or physical adverse effects. The study reports an outbreak of SARS-CoV-2 transmission on the Cornell campus, despite 97.9% of staff and students being vaccinated, and 98.6% of positive tests being in the vaccinated. Staff and students were tested weekly in what is euphemistically called ‘free’ testing – though of course someone ultimately pays for this mass testing – a policy that the WHO explicitly warned against in pandemic planning guidance prior to 2020, including as recently as 2019.
As attested by the CDC, severe COVID-19 is very rare in young adults. Previous meta-analyses of masking for respiratory viruses (e.g. CDC and the Cochrane collaboration) also show low impact, while studies of lockdown impact have shown little benefit. Therefore, the apparent failures on Cornell’s campus are predicted by previous knowledge and could logically have been presented as such. Three years ago, they probably would have been. However, in the brave new world of sponsored publications and business consolidation, the following pearls made it through the editorial and review process:
“While vaccination protected against severe illness, …” but the population was mostly young and the Omicron variant has low severity. In healthy young adults, the expected rate of severe disease is minimal. Though few unvaccinated people were present, this minority actually appeared to have a lower rate of recorded infection. Shouldn’t we be asking whether vaccination is making infection, if not severity, more likely?
“The de-densification (ie. distancing) process decreased student cases (sic) numbers,” But the epidemic curve looks typical for Omicron elsewhere. In a confined population, with a highly transmissible respiratory virus, we would expect a rapid increase followed by rapid decrease in the epidemic curve – and this is exactly what transpired.
Here we have a paper demonstrating a mass failure of vaccine and non-pharmaceutical interventions to control a respiratory virus pandemic, very much in line with orthodox understanding from 2019 and before. It provides the data, even demonstrating a possible (though poorly evidenced) worse outcome for the vaccinated, and then concludes with no evidence whatsoever that the vaccines prevented severe disease, and NPIs halted an outbreak. It is plausible that they all contributed, but equally plausible that they did not. All we can say is that they did not stop transmission, and an outbreak occurred in the presence of very high vaccine coverage and a mask mandate.
Once, the medical profession had the confidence and faith in itself to call a spade a spade, without fear of reprisals. We now live in a world where stating the obvious may be an inhibitor to gaining publication, and can certainly result in major journals attempting to disparage and vilify those with differing opinions. These are echoes of previous times, when medicine played an important role in failing to oppose – or even leading – societal degeneration. As a profession, we should be worried and we should rethink our role, the role of evidence, and the role of those we entrust with sharing it.

Dr David Bell
David is a clinical and public health physician with a PhD in population health and background in internal medicine, modelling and epidemiology of infectious disease. Previously, he was Director of the Global Health Technologies at Intellectual Ventures Global Good Fund in the USA, Programme Head for Malaria and Acute Febrile Disease at FIND in Geneva, and coordinating malaria diagnostics strategy with the World Health Organization.




